Diabetic Foot Care: 5 Ways to Prevent Complications
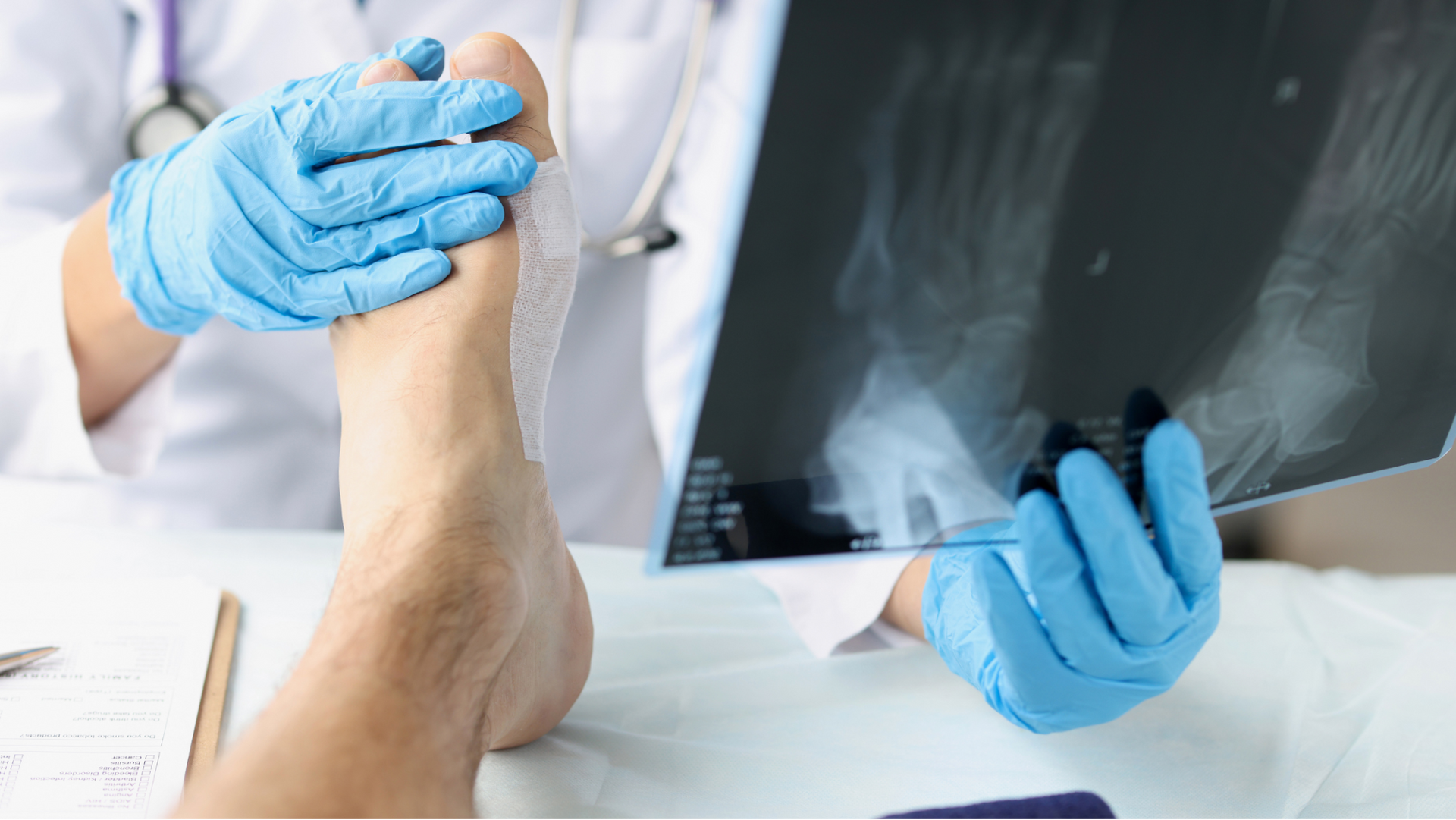
Diabetic foot care is a preventive health practice involving daily self-inspections, specialized footwear, and professional podiatric monitoring. It is essential for individuals with diabetes because high blood sugar causes nerve damage (neuropathy) and poor circulation, which prevent minor injuries from healing, leading to severe infections , ulcers, and potentially amputation.
Why is diabetic foot care so important?
Managing diabetes is a multifaceted challenge, and the feet are often the most vulnerable part of the body. The fundamental reason diabetic foot care carries such weight lies in the intersection of two physiological complications: neuropathy and peripheral vascular disease. When blood glucose levels remain elevated over time, they chemically damage the delicate fibers of the peripheral nerves. This condition, known as diabetic neuropathy, often begins as a tingling or burning sensation but eventually leads to a complete loss of feeling.
Without the ability to feel pain, a patient might walk for miles with a small pebble in their shoe or a blister forming on their heel without ever noticing. Under normal circumstances, pain acts as a biological alarm system, forcing us to stop and address an injury. In a diabetic patient, that alarm system is silenced. Consequently, a minor scrape can quickly escalate into deep wounds because the patient continues to put pressure on the injured area.
Furthermore, diabetes affects the circulatory system. High sugar levels cause the walls of the blood vessels to become thick and less flexible, a process that restricts blood flow to the extremities. Since blood carries the oxygen and nutrients necessary for tissue repair, a lack of circulation means that even a well-cleaned wound will struggle to heal. This combination of "not feeling the injury" and "not being able to heal the injury" creates a perfect storm where minor issues become life-threatening complications. Regular visits to Family Foot & Ankle Specialists are the first line of defense in monitoring these changes before they become irreversible.
How can I protect my feet daily?
Creating a rigid daily routine is the most effective way to mitigate the risks associated with diabetes. Because you cannot rely on your sense of touch, you must rely on your sense of sight. Every evening, you should perform a comprehensive foot inspection in a well-lit room. If you have mobility issues, use a mirror on the floor or ask a family member for assistance. You are looking for redness, swelling, blisters, or any change in skin color. Even a small warm spot can indicate the beginning of an internal infection.

In addition to inspections, hygiene is paramount. Use the following five steps to maintain skin integrity:
- Wash your feet daily in lukewarm (not hot) water using mild soap.
- Dry your feet thoroughly, especially between the toes, to prevent fungus toenails .
- Apply a moisturizing lotion to the tops and bottoms of the feet, but never between the toes.
- Always wear moisture-wicking, seamless socks to reduce friction and keep skin dry.
- Never walk barefoot, even inside your home, to avoid accidental punctures or scrapes.
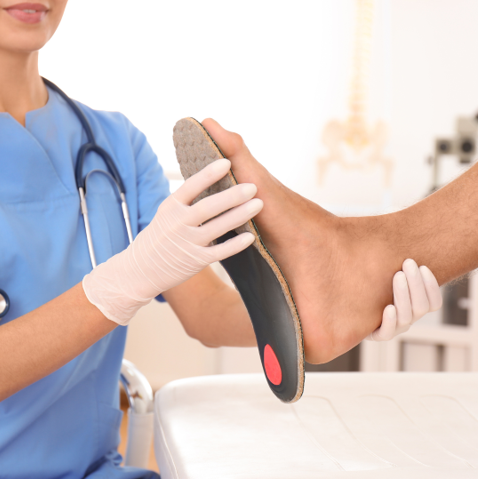
Selecting the right footwear is also a critical component of diabetic foot care . Shoes should be purchased late in the afternoon when your feet are at their largest due to natural swelling. Look for shoes with a deep toe box that doesn't pinch the toes, as compression can lead to bunions or hammertoes . The goal is to eliminate any "hot spots" where the shoe rubs against the skin. If you have significant deformities or high-risk factors, our team may recommend custom orthotics or specialized diabetic shoes to redistribute pressure away from vulnerable areas.
Common Foot Problems for Diabetics
Diabetes changes the way the skin and nails behave. Because the sweat and oil glands in the feet stop working efficiently due to nerve damage, the skin can become extremely dry and prone to cracking. These cracks, or fissures, provide a doorway for bacteria to enter the body. When bacteria invade, the risk of cellulitis or a deep-tissue infection skyrockets.
Patients also frequently deal with calluses and corns . While these might seem like minor cosmetic annoyances to others, for a diabetic, a callus is a significant threat. Underneath a thick layer of dead skin, the pressure of walking can cause the underlying tissue to break down, forming a hidden ulcer. You should never attempt to trim a callus or corn yourself with a razor or over-the-counter "medicated" pads, as these chemicals can burn the skin and lead to a wound. Professional debridement at a podiatry office is the only safe way to manage these growths.
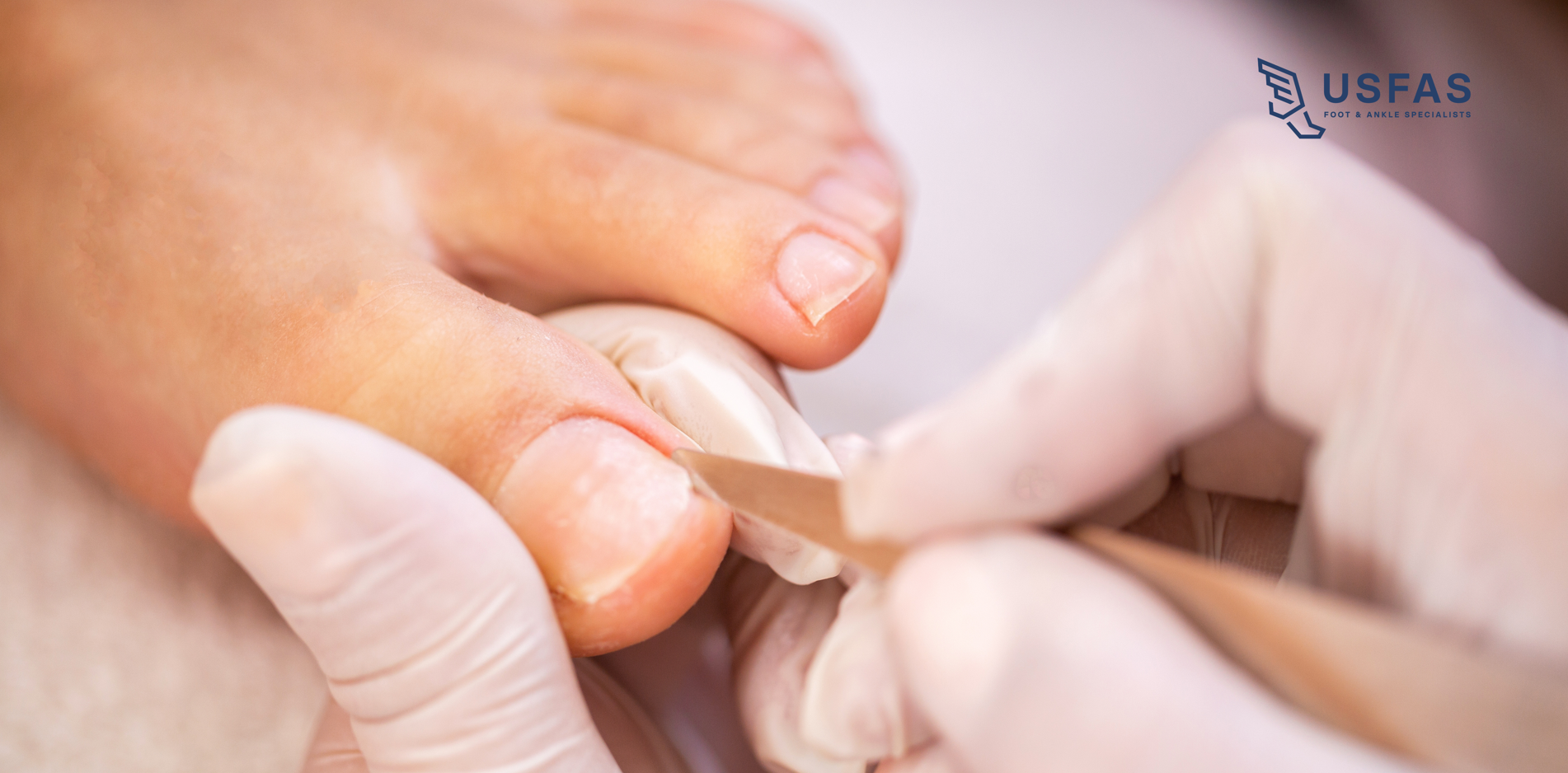
Ingrown toenails are another common concern. In a healthy individual, an ingrown nail is painful and requires a minor procedure. In a diabetic, the same ingrown nail can lead to a localized infection that the body cannot fight off, potentially spreading to the bone (osteomyelitis). Similarly, fungus toenails can cause the nail to become brittle and sharp, which may inadvertently cut the surrounding skin. Regular maintenance by a professional ensures that nails are trimmed safely and any signs of infection are caught early.
What should I look for during a foot inspection?
When performing your daily check, you should be a detective for your own health. Any change, no matter how subtle, is worth noting. Look for changes in temperature; if one foot feels significantly warmer than the other, it may indicate inflammation or infection. Look for changes in the shape of your foot. A condition called Charcot foot can occur when the bones in the foot weaken and shift, causing the arch to collapse. This requires immediate immobilization to prevent permanent deformity.
Pay close attention to your toenails. Discoloration, thickening, or crumbling are signs of a fungal infection that needs treatment. Also, check for "drainage" on your socks. If you notice a yellow or clear stain on your socks, it means a wound has opened even if you don't feel pain. This is a medical emergency for a diabetic patient and requires a visit to Family Foot & Ankle Specialists immediately.
Professional Support at Family Foot & Ankle Specialists
At our offices in Ashburn , McLean , Fairfax , and Reston , we provide advanced diagnostic and treatment options tailored to diabetic patients. We use state-of-the-art technology to assess your circulation and nerve function. If you are struggling with a non-healing wound, we offer specialized therapies such as MLS Laser therapy to stimulate cellular repair and EPAT to increase blood flow to the area.
Our team, including Dr. Richard S. Mendelsohn and Dr. Michael Petranek , works collaboratively with your primary care physician and endocrinologist. We believe in a proactive approach—treating the small issues today so they don't become the surgeries of tomorrow. Whether it is routine nail care or complex wound management, our goal is to keep you active and on your feet.
Summary of Diabetic Foot Care Best Practices
Maintaining your mobility while living with diabetes requires a commitment to vigilance and professional partnership. By understanding that your feet need extra attention due to the hidden effects of neuropathy and poor circulation, you can prevent the majority of complications before they start.
Key Takeaways for Your Health:
- Inspect daily: Use mirrors or help from others to see every part of your foot.
- Prioritize professional care: Schedule regular check-ups even if your feet feel fine.
- Choose footwear wisely: Never go barefoot and wear properly fitted, diabetic-friendly shoes.
- Moisturize carefully: Keep skin supple to avoid cracks but keep the area between toes dry.
- Act quickly: Contact a podiatrist immediately if you notice redness, swelling, or drainage.
If you have questions about your foot health or need a comprehensive diabetic foot exam, contact us today to schedule an appointment at one of our Northern Virginia locations. We are here to help you navigate your journey with diabetes safely and comfortably.